
It goes without saying that before you get your hands on the probe, you need to read up on the manufacturer make and model of the ultrasound system you have in practice. There will be a handbook (or 4 or 5 for some systems!), which will have been supplied at the time of purchase and installation. Like cars, there are lots of common controls, but each manufacturer will have different design features and recommendations which you should take note of, in particular the safety and infection prevention and controls sections. It’s important not to put your patient or yourself at risk in any way when you embark on a scan.
For the success of this training and mentorship programme, you also need to watch the first online video module from ‘The Full Monty’ course to get an underpinning appreciation of how an ultrasound image is formed, how ultrasound interacts with soft tissue and an initial understanding the basic ultrasound controls and how they impact on the image. If you haven’t done this then stop right there and start the video course!
Assuming you now have a reasonable understanding of the way in which our images are formed and which controls do what, you need to select the right probe for the scan type required.
Which Probe?
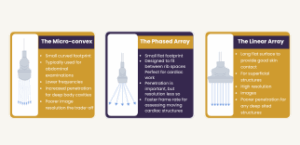
The best suited transducer for medium and large canine abdominal patients, is the low to mid frequency range microconvex one, and for smaller dogs or feline patients, whenever possible, the higher frequency linear array.
Now you need to know how to hold the probe!
Probe Grip
The technique employed for each of the 8-Steps will require you to hold your probe in the most comfortable manner possible (to avoid injury to you!) and in a way we have recognised is best to help you locate and assess the specific structures included in that step. This technique advice that is not written in stone, it’s advice, but we’ve tried it for decades and it works! You need to do what feels right for you, but if you struggle to find the structures we are discussing in any particular step, revert back to our technique suggestions and give it a go!
There are two ways to hold an ultrasound transducer:
The Pencil Grip – thumb underneath the probe

This grip is perfect for scanning the uppermost aspect of the patient (assumed to be lying in the right lateral recumbency position!) as it allows you to rest the heel of your hand on the patient and still perform large and fine probe movements, angle ventral, dorsal, cranial and caudal in relation to the patient, with comfort and precision. So, great for left kidneys, locating the urinary bladder.
You are less likely to use this grip when assessing the patient’s right-sided anatomical structures from the underside of the patient, as it restricts movement and is uncomfortable on the wrist and hand. You are much more likely to adopt the racket grip. If however you still can’t see the right-sided structures in your patient, rather than break your wrist trying to get the image you want, move your patient into the left lateral or dorsal recumbency position and try using either the racket grip or the pencil grip!
The Racket Grip – thumb over the probe

This is the grip you are most likely to use for assessing the midline, central, ventral and right underside anatomical structures of the patient when it is lying in the right lateral recumbency position. You may find at first, that it is difficult to prevent the probe from turning around as you scan because this grip does tend to bulldoze the gel and subsequently make the hand grip slippy! Try wrapping a piece of paper tissue roll around the handle (not the probe contact surface, for obvious reasons!) and this should help you to keep a firm grip on it and prevent it swivelling as you scan.
Correct Transducer Orientation
This is covered in the Fundamentals section of your ‘Full Monty’ online video course, so make sure you watch the demonstrations as this will help you to appreciate why correct probe orientation is so important. Incorrect probe orientation can and will lead confusion as you scan the patient!
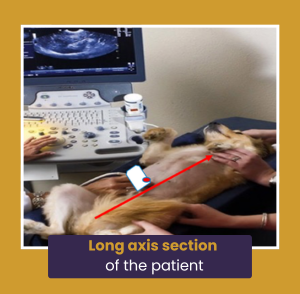
Long axis section of the patient (not necessarily the structure since not all internal structures are aligned along the long axis of the patient!)
Regardless of the way in which the probe is held, the probe orientation marker should be pointing towards the patient head when scanning a patient in long axis. The convention for abdominal scanning is for this orientation marker to correspond to the left hand side of the screen.
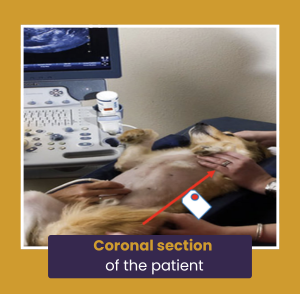
Coronal section of the patient
When scanning in a coronal plane of the patient, the orientation marker should also be pointing towards the patient’s head (think of the coronal plane as a long axis section taken from the side of a patient!)
Short axis section of the patient
When scanning a patient in short axis, on the upper surface of the patient, the abdominal convention is to rotate the probe counterclockwise, which will mean that the orientation marker then points towards the operator. If the patient is being scanned from the ventral surface or underside, then the counterclockwise rotation may mean that the orientation marker points towards the table surface.

Practice turning the probe on the spot, without sliding off that spot, either on a colleague’s forearm or a compliant patient kidney and watch a long structure (vessel or long axis kidney) change from being elongated to rounded in shape. It’s the only way to appreciate the theory.
If you have incorrectly orientated your probe by accident, you will find that the movement on the patient’s skin surface will not reflect the motion seen on the screen (for example, if correctly orientated in long axis, moving the probe to the cranial aspect of the abdomen should result in the image moving towards the left hand side of the screen. If incorrectly orientated, moving the probe towards the patient’s head in long axis, will mean the image on the screen moves in the OPPOSITE direction, towards the caudal abdomen!).
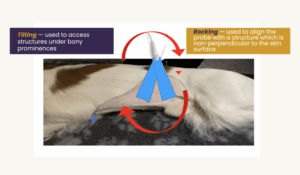
Probe Movements
There are four probe movements to practice and become adept at. They are as follows:


Patient Position
Right Lateral Recumbency Position – First choice for our 8-Step technique as we can usually access all the required abdominal structures as we work clockwise around the abdomen, scanning several structures from more than one approach.
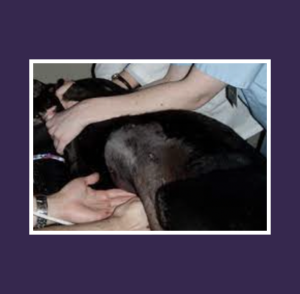
Left Lateral Recumbency Position – It is important to have a flexible and adaptable approach to scanning. We are teaching the 8-Step technique to be performed in the right lateral recumbency position to help standardise a technique and the scan approaches required to fully assess abdominal structures. It is often necessary to alter patient position, especially when body conformation or overlying bowel gas in the GI tract dictate and render visualisation of certain structures technically difficult. Left lateral recumbency position may be helpful for deep right-sided cranial aspect of the liver, the pylorus and descending duodenum etc.

Dorsal Recumbency Position – This position for scanning is often adopted in Europe and mirrors how human patient abdominal scans are initially performed. It is important to appreciate a patient’s respiration parameters though when scanning in this position and not to scan patients with respiratory distress in a dorsal recumbency position. Also any free abdominal fluid present will be more difficult to detect in the dependent aspect of the abdomen when in this patient position.
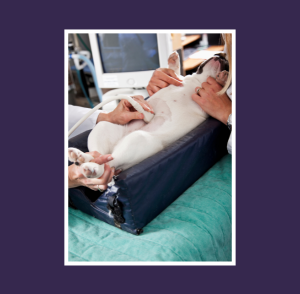

Sternal Position – This position will significantly impact on the full visualisation of abdominal structures as access to the various scan approaches is limited. The position can be used to identify lateral abdominal pathology and free fluid in some clinical scenarios, mainly acute point of care scanning.
Pre-Scan Abdominal Clip
It is important to prepare the patient prior to any routine scans by performing a close clip. The purpose of the clip is twofold. Firstly it is to remove the fur which would otherwise trap air and prevent good ultrasound transmission and secondly, it provides good probe-skin contact enabling easier probe movement over the skin when scanning.
In critical clinical situations, when time is of the essence and a full clip cannot be accommodated, protect the probe with a gel-filled probe cover (gloves will do!), part the fur and apply alcohol as a coupling fluid.
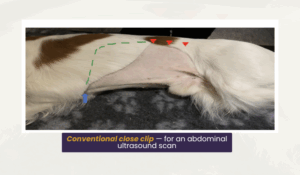
The image below shows a conventional close clip for an abdominal ultrasound scan. As a minimum, the clip should include the ventral abdomen up to the xiphisternal notch, extended cranial along the costal margins and bilaterally along the hypaxial muscle borders.
For deep-chested dogs of when it is technically difficult to assess the far cranial structures, extend the conventional clip (green dotted line) to enable intercostal scanning of the spleen, liver, diaphragm etc rather than simply relying on pressing up and under the rib cage to access structures and assess them in the far field.
Probe Cable and Wheels
If you have done your online video homework, you will know by now that the probe surface contains an arrangement of groups of tiny piezoelectric crystals, these crystals being responsible for ultrasound generation and detection. Each crystal group is connected by a fine micro-wire, both of which are super-delicate and easily damaged.

It’s important that you don’t drop or hit the probe surface as this may permanently damage a small group of crystals, resulting in the loss of ultrasound generation (known as drop-out) at that site, thus compromising the image shown on the screen and interrupting the image frame composition (black lines will be present on the screen, relating to the site of the damaged crystals).
The same is true if the probe cable is damaged by becoming wrapped around the scan cart wheels or being repeatedly run over by a heavy cart! It’s easy to break these fine connections within the cable casing, and this will also cause connection problems and drop out on the screen.

Probes connect into the ultrasound system at the probe ‘port’s once the locking mechanism has been engaged. As you can see below, the fine microwires running within the probe cable casing form an electrical connection at the port end with the internal circuitry of the ultrasound system, as well as with the piezoelectric crystals in the probe surface. Forcing the probe into the port can permanently damage the connections and this will result in considerable image degradation.

Finally, make sure that the probe collar (region where the cable enters the probe handle) is treated with respect – this is a vulnerable part of the probe design and again, connections can be broken if the cable is accidentally pulled away from the probe handle. If you have a cart-based system (one that is designed to be integral with the cart rather than a laptop style), make use of the specially designed probe storage holders, usually to the side of the ultrasound system. Don’t leave the probes dangling!!

Make sure you use manufacturer recommended cleaning materials on your equipment, Failing to do this can lead to irreparable damage and even render the equipment warranty null and void.
If you have a tendency to reach for the alcohol (I mean as a coupling fluid, not a post shift relaxation shot!), then think twice. Alcohol is fine if you cover your probe with a gel-filled glove or a dedicated probe cover, but otherwise with repeated use, the alcohol will have a drying effect on the delicate rubberised probe surface. This can lead to cracking and potentially electrical safety issues.
With probes costing around £5k + VAT each, you can’t afford to use the wrong products!
Now it’s time to put your knowledge into practice!
